When your dog suddenly snaps at a gentle touch, refuses their favorite meal, or withdraws from play, your first thought might be behavioral resistance or anxiety. But what if the real cause is something you cannot see—something silent, persistent, and profoundly affecting their emotional world?
Chronic dental pain in dogs is far more than a physical ailment. It acts as a hidden behavioral driver, reshaping mood, motivation, and social connection in ways that mirror the complex interplay between pain and emotion we see in human neuroscience. Yet, because dogs cannot verbalize their discomfort, this suffering often goes unrecognized, misattributed to temperament issues or training challenges.
Let us guide you through the neurobiological pathways, behavioral indicators, and emotional consequences of dental pain—and explore how understanding this connection can transform the way you support your dog’s wellbeing. 🧡
The Neurobiological Reality: How Pain Rewires the Brain
Chronic Pain and the Limbic System
When dental pain persists day after day, it does not stay localized in the mouth. The pain signals travel through the trigeminal nerve system—the primary pathway for orofacial sensation—directly into deep brain structures that govern emotion, memory, and motivation.
The limbic system, your dog’s emotional control center, becomes profoundly affected by this constant stream of distress signals. Research on chronic orofacial pain in humans reveals that patients experience restricted emotional recognition and difficulty identifying their own feelings—a condition called alexithymia. While your dog cannot tell you they feel emotionally numb, their behavior speaks volumes. The once playful companion who greeted you with enthusiasm may now seem emotionally distant, their spark dimmed by invisible suffering.
How Chronic Dental Pain Affects the Limbic System:
- Emotional Processing Disruption: The amygdala and hippocampus—structures essential for emotional memory and response—become hyperactivated, making your dog more reactive to perceived threats and less able to regulate emotional responses.
- Memory and Learning Impairment: The hippocampus, crucial for forming new memories and learning, operates less efficiently when constantly processing pain signals, making training and adaptation more challenging.
- Motivation Circuit Dysfunction: The nucleus accumbens and ventral tegmental area—your dog’s reward centers—become less responsive to positive experiences, reducing enthusiasm for activities that once brought joy.
- Stress Response Dysregulation: The hypothalamus, which coordinates stress hormones, remains in a state of persistent activation, keeping your dog in a chronic stress state even during calm moments.
This is not simply about tolerating pain. The neurolimbic pain network—the interconnected circuits linking sensation, emotion, and stress response—becomes dysfunctional under chronic pain conditions. What begins as a dental issue evolves into widespread changes in how your dog experiences and responds to their world.
The Inflammatory Connection
Dental disease releases inflammatory cytokines—signaling molecules that do not respect the blood-brain barrier. These chemical messengers travel from infected gums or abscessed teeth directly into your dog’s central nervous system, where they trigger depression-like and anxiety-like states.
Studies on animals with chronic inflammatory conditions demonstrate that these creatures exhibit behavioral changes even without obvious signs of illness. The inflammation itself alters emotional tone, creating a biochemical foundation for behavioral shifts that appear purely psychological.
What Inflammatory Cytokines Do to Your Dog’s Brain:
- Neurotransmitter Disruption: Cytokines interfere with serotonin and dopamine production, the same neurochemicals that regulate mood, motivation, and sense of wellbeing in both humans and dogs.
- Neural Inflammation: These molecules trigger inflammatory responses within brain tissue itself, creating a state of neuroinflammation that affects cognitive function and emotional regulation.
- Blood-Brain Barrier Compromise: Persistent cytokine exposure can weaken the protective barrier between bloodstream and brain, allowing more inflammatory agents to enter neural tissue.
- HPA Axis Activation: Cytokines directly stimulate the stress response system, creating a feedback loop where inflammation drives stress, and stress amplifies inflammation.
Your dog is not choosing to be irritable or withdrawn—their brain chemistry has been fundamentally altered by persistent oral inflammation.
HPA Axis Sensitization and Stress Reactivity
The hypothalamic-pituitary-adrenal axis—your dog’s central stress response system—becomes sensitized under conditions of chronic pain. Think of it as a fire alarm that becomes increasingly sensitive over time, eventually triggering at the slightest provocation.
When dental pain persists, the HPA axis remains in a state of heightened activation. This produces observable changes in your dog’s behavior: heightened irritability, lowered frustration tolerance, and exaggerated responses to minor stressors. The dog who once tolerated grooming sessions calmly may now snap defensively. The previously patient companion may show sudden aggression when children approach too quickly. Through the NeuroBond approach, trust becomes the foundation of learning—but chronic pain erodes that neurobiological capacity for calm connection, making even familiar interactions feel threatening.
Behavioral Indicators: Reading the Silent Signals
Recognizing the Subtle Signs
Dogs experiencing chronic dental pain rarely yelp or obviously favor one side of their mouth. Instead, they adapt, becoming masters at masking discomfort. You might notice:
Observable Behavioral Changes Indicating Possible Dental Pain:
- Head Shyness and Touch Sensitivity: Your dog flinches or pulls away when you reach toward their face, especially around the muzzle—what appears as sudden behavioral resistance may actually be anticipatory protection against pain.
- Food-Related Changes: Food refusal, selective eating patterns, dropping food repeatedly, chewing only on one side, or preferring soft foods over usual kibble—these are not signs of pickiness but adaptive strategies to minimize suffering.
- Excessive Drooling: Salivation increases with oral inflammation, and you may find wet spots where your dog rests or notice more facial wetness than usual.
- Facial Pawing and Rubbing: Repeated pawing at the mouth or face, or rubbing the face against furniture and carpets indicates localized discomfort your dog cannot verbally communicate.
- Reduced Play Drive: The gradual fading of enthusiasm for play, declining invitations to wrestle or tug, or reduced interest in carrying toys—all activities that become painful when dental disease is present.
- Sudden Defensive Behaviors: Snapping, growling, or air-snapping when approached, especially around meal times or when the face is approached—these represent defensive responses from a sensitized nervous system.
- Changed Sleep Patterns: Difficulty settling, frequent position changes, or preferring to sleep with the head elevated may indicate attempts to find comfortable positions that minimize oral discomfort.
- Halitosis: Truly foul breath odors indicate bacterial overgrowth from dental disease—your nose can detect what your eyes cannot see.
Let us explore these signs in greater depth.
Head Shyness and Touch Sensitivity
Your dog flinches or pulls away when you reach toward their face, especially around the muzzle. What appears as sudden behavioral resistance may actually be anticipatory protection against pain. They have learned that touch near the mouth triggers discomfort, and their nervous system now guards against it reflexively.
Food-Related Changes
Food refusal or selective eating patterns often signal oral pain. Your dog may show interest in meals but then eat reluctantly, drop food repeatedly, chew only on one side, or preference soft foods over their usual kibble. Some dogs develop the habit of tilting their heads while eating or moving food to the back of their mouth to avoid painful teeth. These are not signs of pickiness—they are adaptive strategies to minimize suffering.
Drooling and Facial Pawing
Excessive salivation and repeated pawing at the mouth or face indicate localized discomfort. Dogs cannot consciously process why their mouth feels wrong, only that something needs attention. The pawing behavior represents an instinctive attempt to resolve an internal sensation they cannot understand or communicate.
Reduced Play and Social Withdrawal
Perhaps the most heartbreaking indicator is the gradual fading of joy. Play requires physical engagement—wrestling, tugging, carrying toys in the mouth—all activities that become painful when dental disease is present. Your dog may begin declining invitations to play, not from depression in the emotional sense, but because their brain has learned to associate these activities with pain. The Invisible Leash reminds us that awareness, not tension, guides the path—but chronic pain creates an invisible barrier between your dog and their natural joy, one built from protective avoidance rather than conscious choice.
Sudden Defensive Behaviors
Snapping, growling, or air-snapping when approached can emerge seemingly overnight. These behaviors are not dominance displays or obedience failures. They represent defensive responses from a nervous system overwhelmed by persistent nociceptive input—pain signals that have sensitized your dog’s threat detection systems, making them hypervigilant and reactive.
The Misattribution Problem
Here lies the critical welfare issue: how frequently these pain-driven behaviors are misinterpreted as temperament problems, anxiety disorders, or training failures. Without understanding the neurobiological foundation, well-meaning owners and even some trainers may implement behavioral modification strategies that not only fail to address the root cause but potentially worsen the dog’s distress.
Common Misattributions of Pain-Driven Behaviors:
- “My dog is being dominant” → Reality: Head shyness and defensive snapping often stem from anticipatory pain protection, not status-seeking behavior.
- “My dog has separation anxiety” → Reality: Distressed vocalizations and destructive behaviors may reflect overall anxiety amplified by chronic pain-induced stress system dysregulation.
- “My dog is stubborn or uncooperative” → Reality: Food refusal and training resistance frequently indicate that engaging in these activities triggers oral discomfort.
- “My dog is aggressive” → Reality: Sudden defensive behaviors represent a sensitized nervous system responding to perceived threats, not an inherently aggressive temperament.
- “My dog is depressed or lazy” → Reality: Reduced play drive and social withdrawal reflect suppressed SEEKING and PLAY systems caused by persistent pain signals.
- “My dog needs more discipline” → Reality: Inconsistent behavior and “disobedience” often indicate cognitive distraction from pain, not willful defiance.
A dog punished for food guarding behaviors driven by oral pain learns that humans cause additional stress during already painful moments. A dog labeled “dominant” for head-shy behaviors becomes further anxious about human interactions. The biopsychosocial pain model emphasizes that behavioral changes are manifestations of both physical and emotional discomfort—to address only the behavior while ignoring the pain is to treat the symptom while the disease progresses. 🧠

Breed and Structural Considerations
While comprehensive research on breed-specific predispositions to silent dental suffering remains limited, certain anatomical factors warrant consideration.
Breeds and Structural Factors That May Increase Dental Pain Risk:
- Brachycephalic Breeds: Bulldogs, Pugs, Boston Terriers, and Shih Tzus with compressed jaw structures may experience dental crowding, misalignment, and increased pressure on specific teeth.
- Small and Toy Breeds: Chihuahuas, Yorkshire Terriers, Maltese, and Pomeranians often have dental crowding in small mouths, leading to trapped food particles, tartar buildup, and early-onset periodontal disease.
- Long-Nosed Breeds: Greyhounds, Collies, and Dobermans may develop unique wear patterns and are sometimes prone to specific dental abnormalities that cause chronic low-level discomfort.
- Breeds with Genetic Jaw Issues: Certain lines of German Shepherds, Boxers, and other breeds may carry genetic predispositions to malocclusion (improper bite alignment) causing abnormal pressure points.
- Breeds Prone to Autoimmune Conditions: Dogs predisposed to immune-mediated diseases may develop oral manifestations like chronic ulcerative stomatitis or immune-mediated dental resorption.
These dogs might show even subtler behavioral changes because their entire life experience includes some degree of oral discomfort—they have no pain-free baseline for comparison. Understanding breed-specific vulnerabilities helps you become a more vigilant observer of your individual dog’s oral health.
Emotional and Social Consequences: The Ripple Effect
The Erosion of Social Bonds
The relationship between chronic pain and social behavior runs deeper than simple avoidance. Research on oxytocin—the bonding hormone—reveals that this neurochemical normally dampens activity in brain regions associated with negative emotions, particularly the amygdala. Oxytocin facilitates trust, promotes affiliative behaviors, and enables the positive social connections that make the human-dog bond so profound.
Chronic dental pain potentially interferes with oxytocin function. Your dog’s reduced tolerance for handling, decreased interest in petting, and withdrawn behavior during social interactions reflect not a loss of love, but a neurobiological inability to access the positive emotional states that normally make these interactions rewarding. Moments of Soul Recall reveal how memory and emotion intertwine in behavior—a dog who once felt joy during face touching now recalls only discomfort, and their nervous system protects them by creating emotional distance.
The affective neuroscience framework describes fundamental emotional systems—SEEKING, PLAY, FEAR, PANIC, CARE, RAGE, and LUST. Chronic pain persistently activates the FEAR and PANIC systems while simultaneously suppressing SEEKING and PLAY drives. Your dog’s reduced enthusiasm, lack of curiosity, and decreased playfulness represent not behavioral choices but shifts in fundamental motivational circuitry driven by unrelenting pain signals.
Cognitive Impact and Learning Challenges
Training sessions become frustrating for both dog and human when chronic pain is present. Pain acts as a cognitive distractor, consuming mental resources that would otherwise support attention, processing, and memory formation. The limbic system—crucial for learning and memory consolidation—functions suboptimally when constantly processing pain signals.
You might notice your previously responsive dog seems unable to focus, fails to retain training progress, or shows inconsistent performance. Their motivation to work for rewards diminishes because the brain’s reward system operates inefficiently under chronic pain conditions. Food rewards lose their appeal when eating hurts. Play-based reinforcement fails when movement triggers discomfort. Even social rewards feel less rewarding when the neurochemistry of bonding has been compromised.
This is not disobedience or stubbornness. This is a brain trying to learn while simultaneously managing a persistent internal crisis. The same neural circuits that support working memory and attention regulation are being recruited to process and modulate pain, leaving insufficient cognitive capacity for new learning.
Behavioral Setbacks and Recovery Potential
The encouraging news embedded in this difficult reality is that behavioral changes driven by pain are potentially reversible. Human medicine demonstrates that addressing both physical pain and psychological state produces superior outcomes. Patients who receive pain management alongside emotional support show faster healing, reduced anxiety, and better functional recovery.
For your dog, this means appropriate dental treatment—whether scaling and polishing, tooth extraction, or management of oral inflammation—combined with gentle emotional reconditioning can facilitate behavioral recovery. The brain’s remarkable neuroplasticity allows new, positive associations to form when pain no longer dominates the neural landscape.
Mindfulness-based interventions for chronic pain in humans show measurable reductions in both pain perception and emotional symptoms. While we cannot teach dogs formal mindfulness, we can create similar conditions: calm environments, predictable routines, gentle reintroduction to previously painful activities, and consistent positive experiences that allow the nervous system to learn safety again. This approach, grounded in emotional synchrony and gradual desensitization, helps rewire the neural pathways that pain has altered, allowing your dog to rediscover trust and engagement.
Silent. Sharp. Misread.
Pain changes personality. Dental discomfort doesn’t bark—it whispers through withdrawal, irritability, or sudden defensiveness. What looks like attitude is often agony trying to stay unseen.
Inflammation rewires emotion. Oral infection floods the body with cytokines that cross into the brain, dulling joy and heightening stress. Mood shifts aren’t behavioral flaws—they’re biochemical echoes of chronic pain.


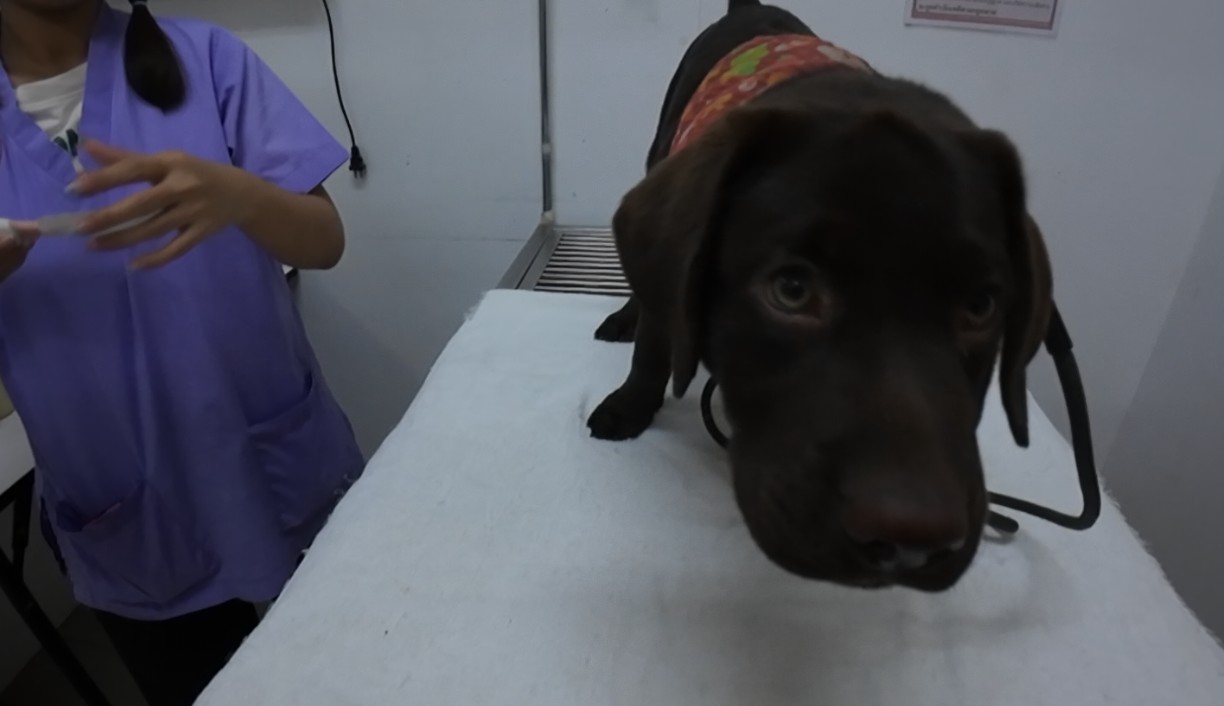
Relief restores relationship. When pain subsides, connection returns. Gentle handling, veterinary care, and renewed trust reawaken calm, proving that healing the mouth can heal the mind.
Clinical and Welfare Implications: A Call for Integration
The Case for Routine Dental Screening in Behavioral Evaluations
Given the profound connections between oral pain, emotional state, and behavioral expression, any comprehensive behavioral evaluation should routinely include thorough dental examination. This is not merely good practice—it is an ethical imperative.
When a dog presents with unexplained aggression, food refusal, training resistance, or social withdrawal, the differential diagnosis must include dental pain. To proceed with behavioral modification protocols without first ruling out pain as a causative factor risks prolonging suffering, implementing inappropriate interventions, and fundamentally misunderstanding the animal’s experience.
Veterinary behaviorists increasingly recognize this connection, but the message must reach general practitioners, trainers, and owners. A simple oral examination—checking for tartar accumulation, inflamed gums, loose teeth, oral masses, or asymmetric wear patterns—takes minutes but can reveal the hidden driver behind months of behavioral challenges.
The Welfare Cost of Underdiagnosis
The chronic underdiagnosis of dental pain in companion dogs represents a significant welfare crisis, though one that remains largely invisible. Consider the cumulative burden:
The Welfare Cost of Underdiagnosis
The chronic underdiagnosis of dental pain in companion dogs represents a significant welfare crisis, though one that remains largely invisible. Consider the cumulative burden:
The Multifaceted Welfare Impact of Unrecognized Dental Pain:
- Chronic Emotional Distress: Day after day of persistent pain creates anxiety-like and depression-like states, diminishing quality of life and draining emotional bandwidth needed to fully engage with experiences that should bring joy.
- Impaired Social Functioning: Emotional distance develops between dog and human, capacity to express and recognize emotional states reduces, and affiliative behaviors gradually erode—representing profound losses in the foundational human-dog relationship.
- Behavioral Deterioration and Mislabeling: Pain-driven behaviors get labeled as aggression, dominance, or anxiety, leading to training approaches that worsen the situation through punishment, isolation, or intensive protocols for an already overwhelmed brain.
- Cognitive Compromise: Inability to learn efficiently, engage with enrichment, or adapt to environmental changes significantly limits the dog’s capacity to experience the full richness of their mental capabilities.
- Progressive Physical Suffering: Untreated dental disease advances, with infection potentially spreading to jaw bones, entering the bloodstream, and affecting distant organs including heart, liver, and kidneys.
- Reduced Quality of Life Across Domains: Pain affects sleep quality, appetite, exercise tolerance, stress resilience, and overall life satisfaction—creating cumulative suffering across every aspect of daily existence.
- Compromised Human-Animal Bond: The relationship strain from misunderstood behaviors, failed training attempts, and the dog’s reduced capacity for affection creates distance and frustration on both sides of the bond.
These factors collectively represent a significant compromise to the dog’s physical, emotional, and social welfare. The suffering is not merely about tolerating discomfort—it is about existing in a diminished state across all dimensions of wellbeing.
🦷 Dental Pain as a Hidden Behavioral Driver in Dogs
Understanding the invisible connection between oral discomfort and behavioral changes 🧠
When aggression, withdrawal, or training resistance might signal chronic pain
🧬 The Neurobiological Reality
How Dental Pain Rewires the Brain
Chronic dental pain doesn’t stay localized in the mouth. Pain signals travel through the trigeminal nerve directly into your dog’s limbic system—their emotional control center—profoundly affecting mood, memory, and motivation.
The Inflammatory Cascade
Dental disease releases inflammatory cytokines that cross the blood-brain barrier, directly triggering depression-like and anxiety-like states. Your dog isn’t choosing to be irritable—their brain chemistry has been fundamentally altered by persistent oral inflammation.
HPA Axis Sensitization
Chronic pain sensitizes your dog’s stress response system, lowering their threshold for reactivity. The fire alarm becomes so sensitive it triggers at the slightest provocation—explaining sudden defensive behaviors, heightened irritability, and lowered frustration tolerance.
🔍 Recognizing the Silent Signals
Behavioral Indicators You Might Miss
Dogs experiencing dental pain rarely yelp or obviously show discomfort. Instead, watch for:
- • Head shyness and flinching when face is approached
- • Food refusal, dropping food, or chewing on one side only
- • Excessive drooling and facial pawing
- • Gradual withdrawal from play and social interaction
- • Sudden snapping or defensive behaviors without obvious cause
- • Changes in chewing patterns or toy preferences
The Misattribution Problem
Pain-driven behaviors are frequently mislabeled as “dominance,” “stubbornness,” or “anxiety.” A dog punished for food guarding caused by oral pain learns that humans create additional stress during already painful moments—compounding suffering and eroding trust.
💚 Pathways to Recovery
Comprehensive Dental Treatment
Professional dental cleaning, selective extractions when necessary, and multi-modal pain management address the physical source. Many owners report their dog “comes back to themselves” after treatment—the personality obscured by pain re-emerges as the nervous system is released from constant distress.
Emotional Reconditioning
Physical treatment alone addresses only half the equation. Gentle desensitization and systematic reintroduction of previously painful experiences allows your dog’s brain to learn safety again. Through the NeuroBond approach, trust becomes the foundation—but this trust must be rebuilt through consistent, pressure-free positive experiences.
Rebuilding Social Connection
As pain resolves, oxytocin function normalizes, allowing the bonding system to reengage. Create opportunities for low-pressure social interactions—parallel activities without demands allow nervous system regulation through proximity. Watch for signs of reengagement: soft eye contact, voluntary approaches, and relaxed body language during interactions.
⚠️ The Welfare Crisis of Underdiagnosis
The Hidden Cost of Missed Pain
Chronic underdiagnosis of dental pain creates cascading welfare impacts:
- • Persistent emotional distress diminishing quality of life daily
- • Impaired social functioning and erosion of the human-dog bond
- • Behavioral deterioration leading to inappropriate interventions
- • Cognitive compromise affecting learning and environmental adaptation
- • Progressive physical suffering as infection spreads systemically
Behavioral Evaluations Must Include Dental Screening
Any comprehensive behavioral assessment for unexplained aggression, withdrawal, or training resistance should routinely include thorough dental examination. To proceed with behavioral modification without ruling out pain risks prolonging suffering and fundamentally misunderstanding your dog’s experience.
⚡ Quick Reference: Early Detection Checklist
Monitor for these early warning signs:
- • Eating modifications: Favoring one side, dropping food, eating more slowly, preferring soft foods
- • Physical signs: Increased drooling, facial pawing, foul breath odor, head-shy behaviors
- • Behavioral shifts: Reduced play enthusiasm, training resistance, sudden irritability, social withdrawal
- • Defensive responses: Snapping near face, food guarding, reluctance during grooming
Early detection prevents behavioral decline and preserves emotional wellbeing. Schedule veterinary dental examination if any signs appear.
🧡 The Zoeta Dogsoul Perspective
Understanding dental pain as a behavioral driver embodies the essence of what we mean by the Invisible Leash—recognizing that awareness, not force, guides the path to healing. When we honor both the neuroscience of pain and the emotional experience of suffering, we create space for true NeuroBond to rebuild. Those moments of Soul Recall—when your dog rediscovers joy after pain has been addressed—reveal the profound interconnection between body, brain, and behavior.
Your dog’s behavior is always communication. Sometimes it speaks of hidden suffering that deserves recognition, validation, and compassionate intervention. That balance between rigorous scientific understanding and deep emotional awareness—that is where transformation lives.
© Zoeta Dogsoul – Where neuroscience meets soul in dog training
Prevention Through Owner Education
Early detection represents the most effective prevention strategy. Educated owners who understand subtle indicators can seek veterinary care before behavioral decline becomes entrenched. What should you watch for?
Early Warning Signs for Proactive Dental Health Monitoring:
- Changes in Chewing Patterns: Notice if your dog favors one side of their mouth, drops food frequently, takes longer to finish meals, or tilts their head while eating—these subtle shifts often precede obvious pain behaviors by weeks or months.
- Increased Drooling: Saliva production increases with oral inflammation, so if you find wet spots where your dog rests or notice more facial wetness than usual, oral discomfort may be developing.
- Facial Rubbing and Pawing: Repeated rubbing of the face against furniture, carpets, or your legs, along with pawing at the mouth or face, indicates localized discomfort that your dog cannot verbally communicate.
- Halitosis: While “dog breath” is common, truly foul odors indicate bacterial overgrowth from dental disease—your nose can detect what your eyes cannot see in the form of infection and decay producing volatile compounds.
- Behavioral Subtleties: Decreased enthusiasm for chew toys, reluctance to retrieve items, less intense play behavior, or slight increases in irritability often represent early warning signs that something has shifted in your dog’s internal experience.
- Eating Modifications: Preference for soft foods, difficulty with hard kibble or treats, eating more slowly than usual, or showing interest in food but hesitating before eating all signal potential oral sensitivity.
- Touch Sensitivity Changes: Gradual increase in head-shy behaviors, pulling away from collar handling, or reluctance during grooming around the face may indicate developing discomfort.
- Sleep Position Adjustments: Preferring to sleep with head elevated, changing sleep positions frequently, or showing difficulty settling may indicate attempts to find comfortable positions that minimize oral discomfort.
Timely veterinary assessment allows for intervention before pain becomes chronic, before behavioral patterns become ingrained, and before suffering becomes a daily reality. The positive effect of early correction extends beyond physical healing to emotional wellbeing and relational quality. 😊
Understanding the Invisible: A Neurobiological Perspective
Central Sensitization and the Altered Pain Experience
One of the most important concepts in pain neuroscience is central sensitization—the process by which the central nervous system becomes hyperresponsive to pain signals. Repeated nociceptive input from chronic dental disease literally changes how the spinal cord and brain process pain information.
Imagine a neural pathway where, initially, significant stimulation is required to trigger a pain response. With central sensitization, that threshold drops progressively. Eventually, stimulation that would normally register as mild pressure now triggers intense pain. Touch that should feel neutral becomes aversive. Your dog’s nervous system has been recalibrated around suffering, making their entire sensory world more threatening.
This explains why dogs with chronic dental pain may show exaggerated responses to seemingly minor events. Their sensitized nervous system interprets ambiguous stimuli through a lens of threat. A child’s quick movement, a dropped dish, or even your approach with the food bowl—all can trigger defensive responses because their brain has learned to expect pain in situations involving the mouth, face, or food.
The FEAR and PANIC Systems
Affective neuroscience research identifies distinct emotional systems operating beneath conscious awareness. The FEAR system mediates responses to immediate threats, preparing the body for defensive action. The PANIC system responds to social separation and loss, driving attachment behaviors and distress vocalizations.
Chronic pain keeps both systems in a state of persistent activation. Your dog exists in a neurobiological state of ongoing threat detection (FEAR) while simultaneously experiencing reduced social buffering capacity (compromised PANIC system function). They feel both more vulnerable and less able to seek comfort effectively.
How Chronic Pain Affects Core Emotional Systems:
- FEAR System Hyperactivation: Your dog’s threat detection threshold lowers dramatically, making neutral stimuli feel dangerous and causing defensive responses to minor events like sudden movements or unexpected sounds.
- PANIC System Dysregulation: The attachment circuitry that normally provides comfort through social connection becomes less effective, leaving your dog feeling unable to seek or receive emotional reassurance effectively.
- SEEKING System Suppression: The curiosity and exploratory drive that motivates investigation and engagement with the environment diminishes as the brain prioritizes pain management over forward-directed behavior.
- PLAY System Shutdown: Joyful social interaction and rough-and-tumble engagement become neurobiologically inaccessible when chronic pain signals dominate brain activity.
- RAGE System Sensitization: Frustration tolerance drops significantly, and your dog may show irritability or defensive aggression when they feel cornered, overwhelmed, or unable to escape uncomfortable situations.
This dual activation explains the complex emotional presentation of dogs in chronic pain: they are simultaneously hypervigilant for threats and unable to fully engage with the social connections that would normally provide emotional regulation. The trust that should characterize your relationship becomes difficult to access when their nervous system signals that safety is perpetually compromised.
The Suppression of SEEKING and PLAY
In healthy states, the SEEKING system drives curiosity, exploration, and goal-directed behavior. It generates enthusiasm, motivation, and the forward-directed engagement that makes dogs such delightful companions. The PLAY system facilitates joyful social interaction, rough-and-tumble engagement, and the exuberant behaviors that signal wellbeing.
Chronic pain suppresses both systems. When the nervous system prioritizes survival and pain management, drives toward exploration and play become luxuries the brain cannot afford. Your dog’s reduced interest in walks, decreased toy engagement, and general lack of enthusiasm reflect not personality changes but shifts in fundamental motivational neurocircuitry.
Recognizing this helps reframe your understanding. Your dog is not being lazy, stubborn, or depressed in the clinical sense. They are operating with a nervous system that has shifted into survival mode, where joy and curiosity become neurobiologically inaccessible luxuries. 🧡
Pathways to Recovery: Hope Beyond Diagnosis
Comprehensive Dental Treatment
The foundation of recovery is addressing the pain source. This may involve professional dental cleaning to remove tartar and calculus, extraction of damaged or infected teeth, treatment of gingival inflammation, and management of any underlying oral pathology.
Components of Effective Dental Treatment for Behavioral Recovery:
- Professional Dental Cleaning: Ultrasonic scaling removes tartar above and below the gum line, followed by polishing to smooth tooth surfaces and reduce future plaque accumulation.
- Dental Radiographs: X-rays reveal hidden pathology like root abscesses, bone loss, retained root fragments, and internal tooth resorption that cannot be seen during visual examination alone.
- Selective Extractions: Removal of teeth that are damaged beyond repair, severely infected, or causing chronic pain—often the most compassionate choice for resolving persistent discomfort.
- Gingival Treatment: Addressing periodontal pockets, treating inflamed or infected gum tissue, and sometimes performing surgical procedures to restore oral health and reduce inflammation.
- Multi-Modal Pain Management: Using combinations of medications that address pain through different mechanisms—local nerve blocks, anti-inflammatory medications, and systemic pain relief working together to interrupt the pain cycle.
- Antibiotic Therapy: When bacterial infection is present, appropriate antimicrobial treatment reduces infectious load and supports healing of inflamed tissues.
- Post-Operative Care: Soft food diets during healing, pain medication protocols for home use, and follow-up examinations to ensure proper recovery and resolution of discomfort.
Modern veterinary dentistry offers sophisticated pain management protocols. Multi-modal analgesia ensures your dog experiences minimal suffering during and after treatment.
For many dogs, the behavioral transformation following appropriate dental treatment is remarkable. Owners report that their dog seems to “come back to themselves”—the personality that pain had obscured re-emerges as their nervous system is released from constant distress.
Emotional Reconditioning and Gentle Desensitization
Physical treatment alone, while essential, addresses only half the equation. The emotional associations and defensive behaviors learned during painful periods require gentle reconditioning.
This process respects the reality that your dog’s brain has been changed by their pain experience. You cannot simply expect them to immediately trust situations that previously triggered suffering. Instead, systematic desensitization allows gradual relearning.
Steps for Post-Treatment Behavioral Reconditioning:
- Establish a Pain-Free Baseline: Wait until your veterinarian confirms healing is complete and pain medication has achieved therapeutic effect before beginning behavioral work—attempting reconditioning while discomfort persists sets up failure.
- Start Below Threshold: Begin desensitization at intensity levels that produce zero defensive response—if face-touching triggered reactivity, start by simply being present near your dog without reaching toward them.
- Pair with High-Value Rewards: Associate previously painful contexts with genuinely rewarding experiences—deliver treats away from the face initially, gradually moving the reward delivery closer as comfort increases.
- Respect Individual Pacing: Allow your dog to set the speed of progress—some dogs recover trust quickly while others need weeks or months, and pushing too fast reactivates defensive patterns.
- Create Predictable Patterns: Establish clear, consistent sequences so your dog learns what to expect—predictability reduces anxiety and allows the nervous system to relax into new, positive associations.
- Use Minimal Pressure Approaches: Remove all coercion, force, or time pressure from training—your dog must feel genuine agency in choosing to engage rather than feeling compelled.
- Celebrate Small Wins: Recognize and reward tiny improvements like softer eye contact, voluntary approach behaviors, or momentary relaxation during previously stressful activities.
- Monitor for Stress Signals: Watch for subtle signs of discomfort (lip licking, yawning, looking away, body tension) and immediately reduce intensity if these appear—staying below stress threshold is essential for neuroplastic change.
Start with creating consistently positive experiences around previously painful contexts. If face touching triggered defensiveness, begin by simply being present near your dog without reaching toward them. Pair this presence with high-value rewards delivered away from the face. Gradually decrease the distance over multiple sessions, always staying below the threshold that triggers defensive responses.
For food-related anxieties, reintroduce eating as a pressure-free experience. Offer highly palatable foods, allow eating in preferred locations, and remove any time pressure or competition. Let your dog’s brain learn that eating no longer equals pain.
The Invisible Leash reminds us that awareness, not tension, guides the path—in recovery, this means reading your dog’s comfort level moment by moment, never pushing past their capacity, and trusting that small, consistent positive experiences accumulate into neurobiological change.
Rebuilding Trust and Social Connection
Social bonds require feeling safe. Your dog’s previous withdrawal or defensive behaviors emerged because their nervous system could not access the neurochemical states that enable trust and affiliation. As pain resolves, oxytocin function can normalize, allowing the bonding system to reengage.
Create opportunities for low-pressure, positive social interactions. Parallel activities—simply being together without demands—allow nervous system regulation through proximity without pressure. Gentle petting in areas your dog finds comfortable (chest, shoulders, back) rather than the head or face helps rebuild positive touch associations.
Watch for signs of reengagement: soft eye contact, approaching voluntarily, soliciting attention, relaxed body language during interactions. These indicate that emotional synchrony is rebuilding, that your dog’s brain is rediscovering the rewarding quality of social connection. This foundation of trust becomes the basis for all future learning and relationship depth.
Ongoing Monitoring and Maintenance
Recovery is not linear, and dental health requires ongoing attention. Regular home examination of your dog’s mouth, annual professional cleanings as recommended by your veterinarian, and immediate attention to any changes in eating or behavior ensure that pain does not return to dominate their experience.
Many dogs require ongoing management of dental disease, particularly as they age. Recognizing this as a chronic health issue requiring consistent care, rather than a one-time fix, ensures your dog maintains the quality of life they deserve.
That balance between science and soul—that is the essence of Zoeta Dogsoul. Understanding the neurobiology of pain while honoring the emotional experience, implementing clinical interventions while respecting the need for psychological healing, and recognizing that your dog’s behavior always communicates something meaningful about their internal state.
A Holistic Framework: Integrating Body, Brain, and Behavior
The Biopsychosocial Model Applied
The biopsychosocial model of pain recognizes that suffering operates simultaneously across biological, psychological, and social dimensions. For your dog, this means:
Biological: The physical pathology of dental disease, inflammatory processes, nociceptive signaling, and neuroplastic changes in pain processing.
Psychological: The emotional distress, altered motivation, cognitive distraction, and defensive behavioral patterns that emerge from chronic discomfort.
Social: The disrupted human-dog bond, compromised ability to engage in affiliative behaviors, and reduced social buffering capacity.
Effective intervention must address all three dimensions. Dental treatment manages the biological component. Emotional reconditioning addresses the psychological impact. Relationship rebuilding repairs the social dimension. Neglecting any aspect leaves your dog with incomplete healing.
Prevention as the Ultimate Intervention
While this article focuses on understanding and treating dental pain, the most compassionate approach is prevention. Regular dental care—including appropriate chew items, daily tooth brushing when possible, routine professional cleanings, and immediate attention to any oral changes—prevents the suffering cascade entirely.
Prevention requires recognizing that dental health is not separate from behavioral health, emotional wellbeing, or relationship quality. They are fundamentally interconnected, operating through the same neural pathways and neurochemical systems.
The Role of Informed Caregiving
Your role as an informed caregiver extends beyond providing food, shelter, and affection. It includes being an attentive observer, noticing subtle changes, advocating for comprehensive veterinary care, and understanding that behavioral challenges often have medical foundations.
When you view sudden behavioral changes through the lens of potential pain, you become a better advocate for your dog’s wellbeing. You ask different questions, notice different patterns, and seek appropriate help sooner. This informed perspective prevents suffering, speeds recovery, and strengthens the trust between you.
Conclusion: Is This Reality Right for Your Understanding?
Dental pain in dogs represents far more than a localized health problem. It operates as a hidden behavioral driver, profoundly influencing emotional state, social behavior, cognitive function, and overall quality of life through well-documented neurobiological mechanisms.
The chronic underdiagnosis of oral pain contributes to widespread behavioral misinterpretation, inappropriate interventions, and unnecessary suffering. By understanding the connections between persistent nociceptive input, limbic system dysfunction, HPA axis sensitization, and behavioral expression, you gain the tools to recognize when behavior changes signal underlying pain rather than training challenges.
Questions to Ask When Behavioral Changes Appear:
- Has this behavior emerged suddenly or gradually increased? Rapid onset or progressive worsening often indicates an underlying physical cause rather than purely behavioral development.
- Does my dog show increased sensitivity around their head, face, or mouth? Pain localization frequently manifests as touch avoidance in the affected region.
- Have eating patterns, food preferences, or mealtime behaviors changed? Oral pain directly impacts feeding, often before other signs become obvious.
- Is my dog less engaged in activities they previously enjoyed? Reduced play, exploration, or training enthusiasm may reflect suppressed SEEKING and PLAY systems due to chronic pain.
- Do defensive or aggressive responses seem disproportionate to the trigger? Exaggerated reactivity often indicates a sensitized nervous system responding to ongoing internal distress.
- Has my dog’s overall demeanor shifted toward more withdrawn, anxious, or irritable? Emotional tone changes reflect altered neurochemistry from persistent pain and inflammation.
- When was my dog’s last comprehensive dental examination? If more than a year has passed, or if you cannot remember, dental assessment is overdue.
- Would I want to interact enthusiastically if my mouth hurt constantly? This empathy question reframes behavior through the lens of physical experience rather than intentional choice.
The encouraging truth within this difficult topic is that recognition leads to treatment, treatment enables recovery, and recovery allows your dog to rediscover the joy, trust, and connection that chronic pain had obscured. Your dog’s behavior is always communication—sometimes, it is telling you about suffering that deserves recognition, validation, and compassionate intervention.
Through awareness of these neurobiological realities, commitment to regular dental care, and willingness to view behavioral changes as potentially pain-driven, you honor the depth and complexity of your dog’s internal experience. This understanding transforms how you interpret behavior, approach training challenges, and advocate for comprehensive veterinary care.
Did you know that the same neural pathways carrying pain signals also process emotional information, social bonding cues, and learning capacity? Understanding this integration reveals why dental pain influences so much more than physical comfort—it reshapes your dog’s entire subjective experience of life.
Let this knowledge guide you toward proactive dental care, careful behavioral observation, and holistic wellness approaches that honor both the scientific reality of pain neurobiology and the emotional depth of the beings we share our lives with. Your dog cannot tell you in words when something hurts, but their behavior, when understood through an informed lens, speaks clearly.
That balance between rigorous scientific understanding and compassionate emotional awareness—recognizing that behind every behavioral change lies a neurobiological reality, and within every neurobiological reality lives a being deserving of pain-free existence—that is the approach that serves our dogs best. 🧡
Next Steps for Concerned Owners:
If your dog exhibits any of the behavioral patterns discussed—head shyness, food refusal, reduced play, sudden defensiveness, or social withdrawal—schedule a comprehensive veterinary examination including thorough oral evaluation. Early detection prevents behavioral decline, preserves emotional wellbeing, and honors your dog’s fundamental right to comfort.
The strongest relationships are built on mutual understanding, and understanding sometimes requires looking beneath behavior to discover hidden suffering. Your attention to these subtle signals can transform your dog’s life.










